Vision Problems As You Age? You May Be a Candidate For Cataract Surgery
Changes in your eyesight can be unsettling, especially as you get older. Symptoms like cloudy vision or difficulty seeing at night are more than just a sign that you need to update your prescription.
What could be the cause of your new vision problems? For those who are over the age of 60, the answer may be cataracts. As a result of normal aging, cataracts can begin forming at any age. However, by age 65, over 90% of people in the U.S. have cataracts.
If you are experiencing vision concerns related to cataracts, you’re not alone. There’s also an easy solution: the experts at Durrie Vision have a 10-to-15-minute outpatient solution to give you the best vision possible.
Keep reading to learn more about cataracts and whether you are a candidate for refractive cataract surgery at our office.
What Causes Cataracts? How Do They Affect Your Vision?
Cataracts form gradually and are a result of normal aging. Although refractive errors, such as myopia, hyperopia, and astigmatism, stem from the shape of the cornea, lens, and length of the eye, cataracts are a product of the thickening and compression of the crystalline lens inside the eye, which changes the clarity, focus, and light transmission properties.
To understand how an aging lens affects your vision, let’s take a step back and discuss the anatomy of the eye.
Your eye functions much like a camera. The cornea, which is the clear dome at the front surface of your eye, provides the first focusing of light. If the cornea is too steep, too flat, or out-of-round, the light will not be focused on the retina, which is the “sensor” at the back of the eye. These types of refractive errors often develop in adolescence and into early adulthood and are the reason individuals need glasses, contacts, or LASIK surgery to see their best.
The crystalline lens, located behind the iris (the colored portion of the eye), provides the second focus of light. Ideally the cornea and lens together will focus light directly on the retina. In early life, the lens is a flexible structure and acts like a zoom feature to provide near focus. As time passes, however, the lens thickens, resulting in the loss of this zoom usually by the mid-40s.
There are typically three stages of lens deterioration, known as Dysfunctional Lens Syndrome:
- During stage one, people use reading glasses, bifocals, or specialized contact lenses to compensate for the near vision loss. Fast-forward a decade or so, and stage two begins.
- The lens begins losing its clarity. Haze and yellowing of the lens leads to a decrease in vision quality, including nighttime halos and glare and increased need for light to read. During this phase, refractive lens exchange is a surgical option to restore image quality and range of vision before cataracts are fully formed.
- Left untreated, the aging lens progresses into cataracts. Symptoms of cataracts will vary depending on the location and type of cataract change.
Symptoms of Cataracts
- Cloudy vision: Cataracts decrease the amount of light that reaches the retina and can make vision appear generally foggy, less bold or crisp, and less bright.
- Halos and glare: Early peripheral layering of the lens will often cause glare and halos around lights at night or in bright morning or afternoon sun, when light is coming from a more direct angle relative to your line of sight.
- Difficulty seeing at night: Lens clarity will challenge reading in dim light or at night, especially while driving.
- Change in color perception: As the lens ages, it begins to yellow, making whites appear dingy and colors less vibrant.
Other less common symptoms may include:
- Frequently changing eyeglasses prescription
- Double vision
- Loss of contrast
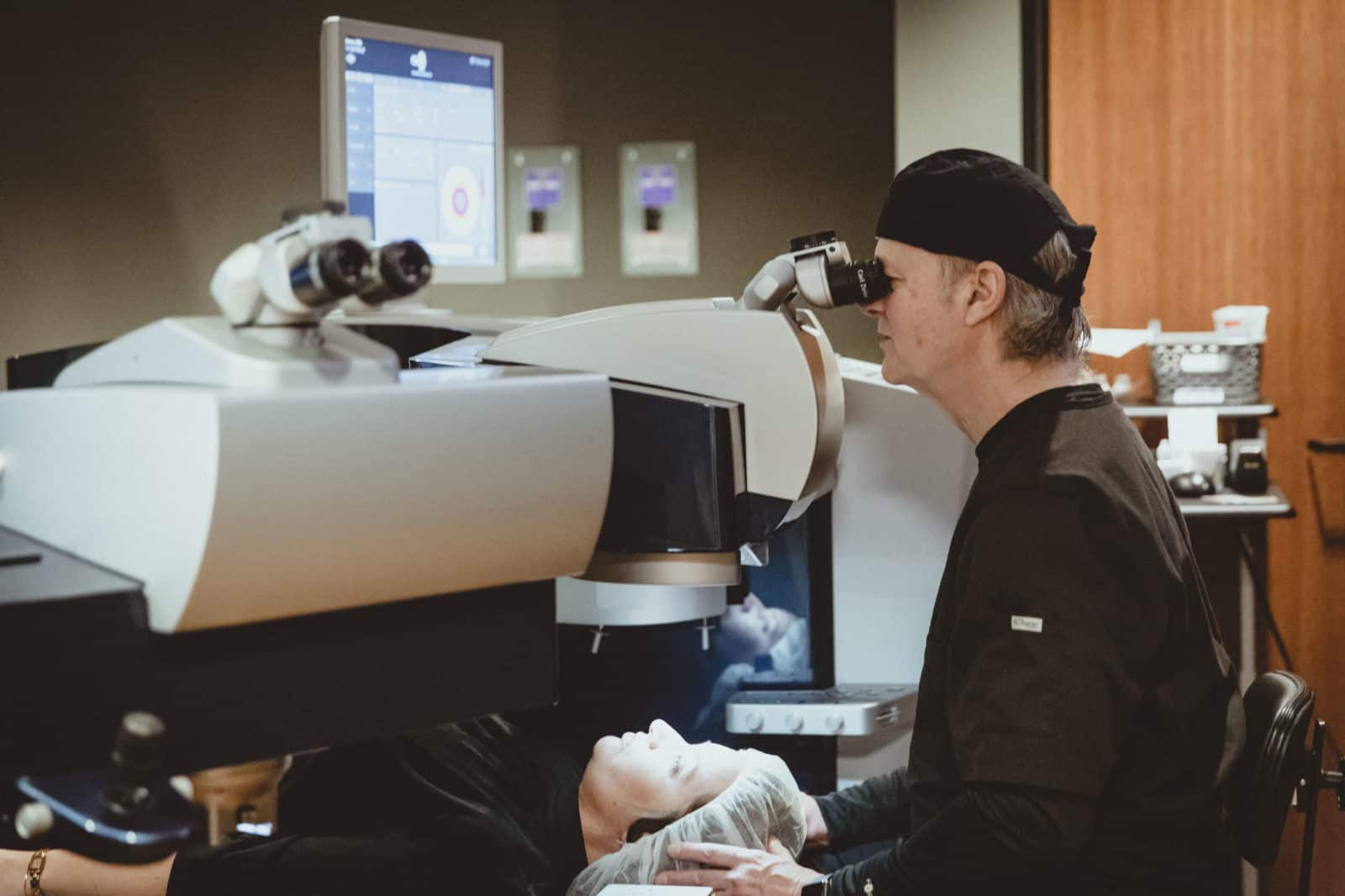
What Does Refractive Cataract Surgery At Durrie Vision Involve?
Refractive cataract surgery from Kansas City’s Durrie Vision is an outpatient procedure, performed one eye at a time, typically a week or two apart. On surgery day, patients should expect to be in our surgery center for 90 minutes, though surgery itself lasts 10 to 15 minutes.
Before surgery, you’ll receive two forms of topical anesthetic and a mild oral sedative to keep you comfortable during the procedure. Next, your refractive surgeon makes a small incision at the edge of the cornea to allow access to the lens. The surgeon removes the lens using gentle ultrasound and aspiration and positions an artificial lens into the eye. Finally, your refractive surgeon seals the incision using a sutureless technique.*
What Does the Refractive Cataract Surgery Recovery Process Look Like?
On the day of surgery, your vision will be blurry due to dilation of the eye and early healing. You will need to attend a postoperative visit the day following surgery. Usually patients notice a dramatic improvement in vision by exam time and are cleared to return to most normal activities (except swimming and heavy-lifting).
You’ll need to use prescription eye drops before and after refractive cataract surgery to promote healing and protect against infection and inflammation. These drops are used for the four weeks following surgery, decreasing usage over time as your surgeon prescribes.
Monitoring your healing and visual progress is key to reaching optimal results, so patients return for examination at one week, one month, and three months postoperatively. Examinations are performed annually or biennially (every two years) thereafter.
What Is the Difference Between Refractive Cataract Surgery and Basic Cataract Surgery?
While both basic cataract surgery and refractive cataract surgery replace the clouding lens with a clear intraocular lens (IOL), only refractive cataract surgery aims to correct all forms of refractive error. The technological improvements in artificial lenses allow Durrie Vision to provide distance, intermediate, and near vision, superb image quality, and contrast sensitivity in both eyes!
Here are the other key differences between refractive cataract surgery and basic cataract surgery:
Refractive Cataract Surgery
- Multifocal, trifocal, extended depth of focus lenses available
- Toric lenses or LRI astigmatism correction standard
- Laser vision correction included postoperatively if needed to optimize vision
- Range of vision provided using IOL technology
Basic Cataract Surgery
- Monofocal lenses only
- No astigmatism correction offered
- Glasses/bifocals used to correct residual refractive error
- Readers or bifocals needed for intermediate/near
How to Choose the Right Lens During Refractive Cataract Surgery
Our doctors spend significant time understanding your needs and setting expectations so you can achieve the best vision possible. With a multitude of lenses available for use, a significant part of optimal visual outcome involves appropriate assessment of your individual optics, your visual potential, and the unique visual demands that correspond to your lifestyle.
The surgeons at Durrie Vision utilize the most advanced diagnostic technology available along with years of expertise with refractive lens technology to customize a treatment plan tailored to your visual needs. Whether it be your occupational needs, your recreational pursuits or your hopes for the future, choosing the right lens is critical to your functionality.
Get Durrie Vision’s Free Consultation for Refractive Cataract Surgery
For over 20 years, our refractive surgeons have been leaders in the field, specializing in the most-advanced techniques in vision correction.
Our primary goal is to help our patients experience life with the best vision possible. The first step in that process is a comprehensive examination. We begin with our signature exam, the Advanced Ocular Analysis.
During your AOA we will perform a series of in-depth, advanced diagnostic tests. Following the testing, a surgeon will examine your eyes, review the tests, and recommend a customized plan to help you reach your visual goals.
As a refractive surgery practice, we perform seven procedures, including laser vision correction and lens implantation using innovative technology for precise and tailored treatment. Our expert staff is here to provide superior service, beginning with your free consultation.
Schedule your free consultation with Durrie Vision, the leading provider of cataract surgery in Kansas City.

Author Bio: Jason E. Stahl, MD
Top Doctors: https://www.castleconnolly.com/top-doctors/jason-e-stahl-ophthalmology-129cc002150
Best Cataract Surgeons: https://bestcataractsurgeons.com/cataract-surgeons/jason-e-stahl/